 Reading Time: 8 minutes
Reading Time: 8 minutesWant to know how far you’ve come? You need to know where you started.
Self-assessments are an important part of the Whole Life Challenge. Measurements at the beginning let you know what kind of progress you’ve made, and provide an objective picture of your health.
The Whole Life Challenge includes three assessment phases.
- Phases 1 and 2 include baseline measurements: weight, waist and hip size, and fitness tests. These are great ways to track improvement, but there’s more to health than these exterior metrics. To have a complete understanding of your health, you have to go further, and take a look at your blood.
- Phase 3 goes inside the body: testing blood lipids and blood glucose, measuring HDL, LDL, triglycerides, hemoglobin A1C, and glucose.
If you’ve never had a blood test, you’re missing an important piece of the health puzzle. It’s especially meaningful if you are about to make significant changes to your diet and exercise routine.
Without a blood test, you can’t know how all the vegetables you’ve been eating have impacted your blood lipids. How has your blood glucose changed after giving up sugar? If you’re exercising and adding muscle, you might not see a change on the scale, but you could see tangible improvement in your blood work.

Remember, “health” isn’t something that just happens on the outside. In fact, it mostly happens on the inside.
But most doctors only test your blood to look at one thing: cholesterol. At the Whole Life Challenge, we believe that isn’t enough. Here are the blood tests we recommend in our Phase 3 Assessments, and why we think they are an essential part of the challenge.
Low-density lipoproteins (LDL) and high-density lipoproteins (HDL) serve an essential function in our bodies—they carry cholesterol to and from the cells. Cholesterol can’t dissolve in the blood, so it has to be transported through the bloodstream by these lipoproteins.
Why are they so different, and why is one “good” and one “bad”?
LDL and HDL differ first by their composition. LDL particles have about 50 percent cholesterol and 25 percent protein. HDL particles are approximately 20 percent cholesterol and 50 percent protein. Protein is denser than fat, so that’s what makes HDL “high-density.”
The other important difference between LDL and HDL is their function. They both transport cholesterol, but deliver it to different parts of the body. LDL particles, which are about half cholesterol, carry cholesterol to cells throughout the body, including your arteries.
HDL particles carry cholesterol away from the heart and other organs and deliver it back to the liver, where it is eliminated from the body. That’s why HDL is considered the “good” cholesterol. Too much LDL is thought to lead to arterial blockage, which in turn can increase the risk of heart disease and stroke. This is how LDL got the “bad” cholesterol name.

Unfortunately, it may not be that simple. Recent research suggests cholesterol causes a health problem only when it is rancid, or oxidized. Cholesterol can become rancid as a result of oxidative stress and free radicals. Oxidative stress happens when your body does not have enough antioxidants to combat free radicals, which are unstable molecules that can damage or create abnormal cells. You’ve probably heard of antioxidants—and they’re yet another reason to eat a variety of whole foods, as vegetables and fruit are rich with them.
Science also suggests it’s not fat that causes harmful cholesterol particles, but sugar. Refined carbohydrates or sugar cause the HDL to go down and triglycerides to go up, and can lead to the small cholesterol particles that build up in the arteries and cause metabolic syndrome or pre-diabetes.
So you can see it’s not as simple as “good” and “bad” cholesterol.
A Little Bit More About Cholesterol
For many years, scientists told us to reduce the “bad” cholesterol in our bodies, we should avoid eating foods that contain cholesterol, like egg yolks, fish oil, animal fats, red meat, and shellfish.
Then, in 2015, there was a major reversal on this thought. The United States government, via its Dietary Guidelines Advisory Committee, altered its stance on cholesterol-laden foods. It said cholesterol was no longer a “nutrient of concern,” and instead changed its focus to foods high in saturated fats, such as fatty meats, whole milk, and butter.
The switch was due to recent science that found the body creates cholesterol in amounts higher than any diet could provide, and that each person processes cholesterol very differently. While there is confusion about the impact of diet when it comes to lowering LDL, exercise does help raise HDL.
The most important thing to take away from all of this, is that measuring your LDL and HDL can give you a more complete picture of your health, and help you see the impact of improving your nutrition, fitness, and lifestyle habits.
Generally, healthy levels are LDL under 100 mg/dL and HDL over 40 mg/dL for a man (over 60 mg/dL for a woman).1
Triglycerides and Free Fatty Acids
The third blood lipid included in the Phase 3 assessment is triglycerides. Triglycerides are the fat in your blood, which provide your cells with energy. Triglycerides are also the source of fatty acids, which your cells need for cell-to-cell communication and also help form molecules important for nerve transmission and inflammatory response.
The Whole Life Challenge recommends testing triglyceride levels along with cholesterol because too much sugar, or refined carbohydrates, drives down the good cholesterol and raises triglycerides, which can lead to heart attacks. Simply testing cholesterol alone will not give you the complete picture of your overall health.

If you have extra fat in your blood, it gets stored in various places in your body, to be used later. If this condition is chronic, you may develop hypertriglyceridemia, or high triglycerides. Elevated triglycerides could be linked to hardening of the arteries or thickening of the artery walls, which increases the risk of heart disease, heart attack, and stroke. High triglycerides are also associated with pancreatitis and sometimes type 2 diabetes.
Losing weight, improving nutrition, limiting alcohol, and exercising are all ways to lower your triglycerides, so if your initial assessment showed unhealthy triglyceride levels, following the WLC could help get that number under control.
A desirable triglyceride level is under 150 mg/dL.2, 3
Hemoglobin A1C and Glucose
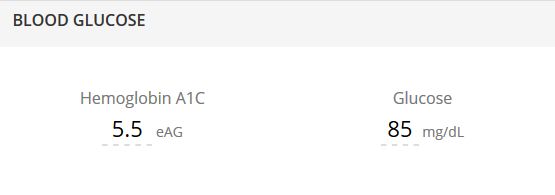
Heart disease is not only linked to cholesterol — blood sugar plays a role as well, which is why it’s important to test the two together. Abnormal blood sugar can be a sign of insulin resistance, when the body’s cells don’t respond normally to insulin and glucose builds up in the blood. It can also be linked to metabolic syndrome, which includes high blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol. Both insulin resistance and metabolic syndrome can lead to cardiovascular disease, so keeping an eye on your blood sugar is as important as monitoring your cholesterol and triglycerides.
We recommend two types of blood sugar testing. A simple blood sugar, or “glucose,” test tells you the amount of glucose in your bloodstream at the instant the blood is drawn. This result can be affected by foods you’ve eaten, stress, medicine you’re taking, or recent exercise.
Glucose tests are helpful, even for non-diabetics, to determine if you are pre-diabetic or if you have impaired glucose tolerance. Seeing how your body reacts to food immediately after consuming it lets you know if that food is generally a good or bad idea for you to consume, or perhaps even if your body is just not in a state where it can deal with additional sugar intake.
The hemoglobin A1C test measures the percentage of red blood cells with a sugar coating. People who have more sugar in their bloodstream will have a higher percentage. Typically used for monitoring diabetics, the A1C test measures the average blood sugar for the past two to three months.
Together, these two blood tests combined give a more complete picture of your blood sugar levels, allowing you to see how your body is handling sugar both over the short term and long term. This could be the difference between your blood sugar being impacted by a single “cheat” meal or chronic metabolic derangement due to consistently unhealthy eating habits.
A person without diabetes should have an A1C level below 5.7 percent. Non-diabetics should have a fasting blood sugar under 100 mg/dL. Generally, before-meal normal sugars are 70 to 99 mg/dL and post-meal numbers should be less than 140 mg/dL.4, 5, 6

Head-to-Toe Health
Good health is achieved by pursuing a variety of healthy habits, and an awareness of how your habits impact your overall health and well-being. Tracking your progress is part of the process, but it is about more than stepping on the scale.
Until you know your cholesterol, triglycerides, and blood sugar, you don’t have a complete picture of your health. Phase 3 measurements give you a peek inside your body, letting you know what changes you need to make for optimum health.
Want to learn more about healthy eating? Join us for the next Whole Life Challenge. You will improve your mind, your body, and your daily habits, leaving you happier, healthier, and in control of your lifestyle. If you’re ready for a change, this is your opportunity. Click below to learn more.
Where to Get Blood Tests Done
Ideally, your primary care physician can order these blood tests for you. But, while laws in a few states expressly prohibit it, in many states you can have blood drawn and tested at private labs or use at-home testing kits